If you have been told that you have carpal tunnel syndrome, you may have also been sent for a Nerve Conduction study and Electromyography to confirm the diagnosis. Another option for diagnosis is to look at the nerve under ultrasound, so let’s discuss the pros and cons of each approach.
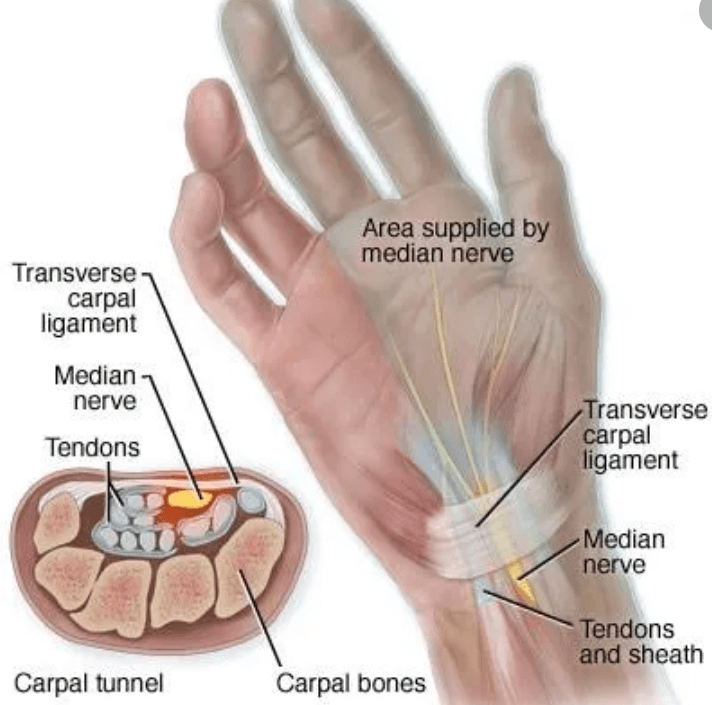
Let’s back up for a moment and define CTS. CTS involves pain, numbness, tingling and weakness in the fingers of the hand or palm. These symptoms sometimes radiate up the forearm and become worse while sleeping or with repetitive activities. CTS occurs when the median nerve, one of the major nerves in the arm, is compressed as it makes its way through the carpal tunnel. This nerve can be compressed or damaged by the transcarpal ligament or the flexor tendons, which lie next to it in the wrist. CTS affects more than 12 million people nationwide and will affect approximately 10% of the population at some point in their lives.
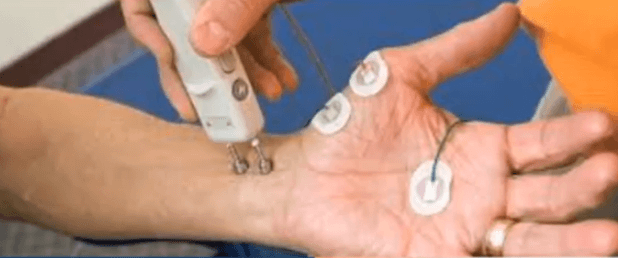
NERVE CONDUCTION STUDY AND ELECTROMYOGRAPHY
The most commonly-performed diagnostic test to confirm CTS is called a Nerve Conduction Study and Electromyography. In this study, electrodes are placed along the path of several nerves in the hand and wrist. Then an electrical signal is sent through the various nerves of the hand and arm so that the speed of the signal along each nerve can be measured. Through this test, the physician can tell if the median nerve is damaged, compared to the other nerves of the hand and wrist. The physician can also tell where damage is likely coming from. The physician will often follow this up by putting a small needle that acts as a microphone into several muscles in the hand and arm to assess the ‘nerve to muscle’ connection. This test is an excellent tool to diagnose carpal tunnel syndrome, but it has its downsides. Unfortunately, the test is often rather uncomfortable for patients and is associated with pain during simulation along the nerve and when needling the various muscles. The electromyography portion of the exam can be useful to distinguish between nerve damage coming from the carpal tunnel and nerve damage coming from the neck.
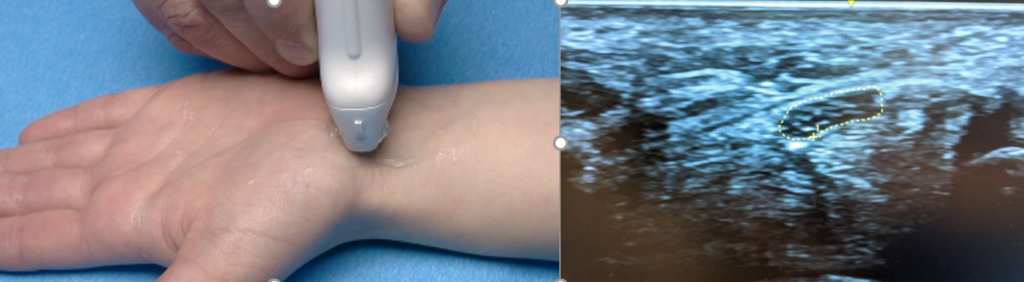
DIAGNOSTIC MUSCULOSKELETAL ULTRASOUND.
By using a musculoskeletal ultrasound machine, a physician can obtain measurements of the cross sectional area of the median nerve at the carpal tunnel. These measurements can tell the physician if the patient has objective evidence of carpal tunnel syndrome in less than a minute. The ultrasound is also cheaper and does not have any pain associated with the procedure.
NERVE CONDUCTION STUDY & ELECTROMYOGRAPHY PROS
- Excellent at diagnosing CTS
- Can distinguish between CTS and nerve damage from the neck well
NERVE CONDUCTION STUDY & ELECTROMYOGRAPHY CONS
- Painful
- Takes 20-30 minutes
- More expensive
ULTRASOUND PROS
- Excellent at diagnosing CTS
- No pain
- Takes 1-2 minutes
- Cheaper
ULTRASOUND CONS
- Does not tell any information about nerves coming from the neck.
RECAP
In general, patients may prefer the no-pain, quick and cheaper approach of diagnosing CTS with the ultrasound vs Nerve Conduction and Electromyography, however some patients with neck issues may benefit more from Electromyography.



